The Importance of Data-driven Decision-making
Google “clinical informatics,” and a number of definitions are revealed. The American Medical Informatics Association and HIMSS (Healthcare Information and Management Systems Society) define it similarly, indicating that clinical informatics—aka health informatics—is the study of using technology and data analytics (or the application of informatics) to improve patient care plans or the effective delivery of care services.
In healthcare, many disciplines have access to mounds of data and analytics that are often used for a variety of purposes. On the supply side, data is used to help drive standardization, eliminate unnecessary variation and lower costs.

“The prevalence of a clinically integrated supply chain is the result of today’s focus on value-based care initiatives,” says HealthTrust’s Chief Medical Officer John Young, M.D., MBA, FACHE. “Achieving the triple aim (intersection of cost, quality and outcomes) requires that previously disparate sources of data come together in response to the new reality of reimbursement models, which are directly tied to patient outcomes. This type of analysis is also key to reducing unwanted variations in care, lowering costs and improving the patient experience.”
“Success in this new reality requires an ability to harness data to understand, predict and manage clinical and operational performance,” says Ed Hickey, MBA, former HealthTrust AVP & data scientist. “Those who do it well will be able to bring new data sources to bear which may accelerate medical research, improve clinical and financial risk projections, reveal new operational efficiencies, or more closely tailor clinical decisions to a patient’s biology and disease state.
“The retail, marketing, manufacturing and transportation industries—even politics—have already incorporated big data techniques into their operating models, and a number of health systems are incorporating it into their research and other initiatives such as population health,” he adds.
What Is ‘Big Data’?
Big data is just another way of referring to analytics, offers Hickey. Both glean intelligence from data and translate it into a business advantage. However, big data is most often viewed from the characteristics of volume, velocity and variety, he adds.
Volume is essentially the amount of data that exists. Velocity—data in motion—is perhaps even more important than volume, as it can become a competitive differentiator. By gathering information in real time, a company can be more agile than its competition. The third characteristic is the variety of forms big data can take. Think about all of the messages, images and videos shared through social media, GPS signals from cell phones and satellites, passive readings from sensors, etc. Unlike information generated from traditional systems, much of this data is unstructured and unwieldy to store and process, Hickey suggests.
Big data and analytics bring vast opportunities, but they also present organizational challenges across a number of areas, including technology and culture.
Technology is a central challenge in using big data. A strong technology foundation entails multiple components, starting with an infrastructure capable of capturing, centralizing and storing a wide range of data. There are then analytical applications that enable people to track key performance indicators, visualize trends and ask questions of the data.
A company’s culture needs to evolve to become more data-driven and insight-based:
• Moving away from acting on instinct and “What do we think?” to instead asking, “What do we know?”
• Connecting people who understand the problems with those who can mine the data for solutions
• Encouraging decision-makers to be overruled by data (e.g., a senior leader conceding when evidence disproves a hunch)
• Asking consistently “What does the data say?” and “How confident are we in the results?”
Data Is Central to Performance
Surprisingly, too often in healthcare, decision-making is not data-driven. A 2016 PwC Global Data and Analytics survey indicated nearly two-thirds of both healthcare and other industry respondents characterized decision-making in their organizations as being “rarely” or “somewhat” data-driven.
Typically, Hickey explains, three types of analytics are utilized to understand, predict and manage operational performance:
Descriptive analytics – dashboards, scorecards and alerts are used to illustrate what happened in the past, but not why it happened or what might change
Predictive analytics – past data is used to model future outcomes (e.g., which patients have the greatest propensity to readmit)
Prescriptive analytics – techniques such as optimization or A/B testing are used to help inform how to do certain activities (e.g., advising a physician on which drug(s) to prescribe for a patient with a certain condition)
“Data-driven organizations typically use more predictive and prescriptive analytics,” Hickey says. The PwC survey revealed, however, that the majority of healthcare organizations are heavily concentrated on the use of descriptive analytics.
HealthTrust’s Clinical Data Solution Evolves
In an effort to further its members’ ability to achieve the triple aim and provide superior care at a lower cost, HealthTrust is utilizing predictive analytics to advance its clinical informatics offering.
Hickey says, “We are increasing the ability to gather data that is oftentimes disparate and siloed (see Figure 1), cleanse and align it, and apply more sophisticated analyses and automated business intelligence reporting through dashboards featuring information requested by HealthTrust members.
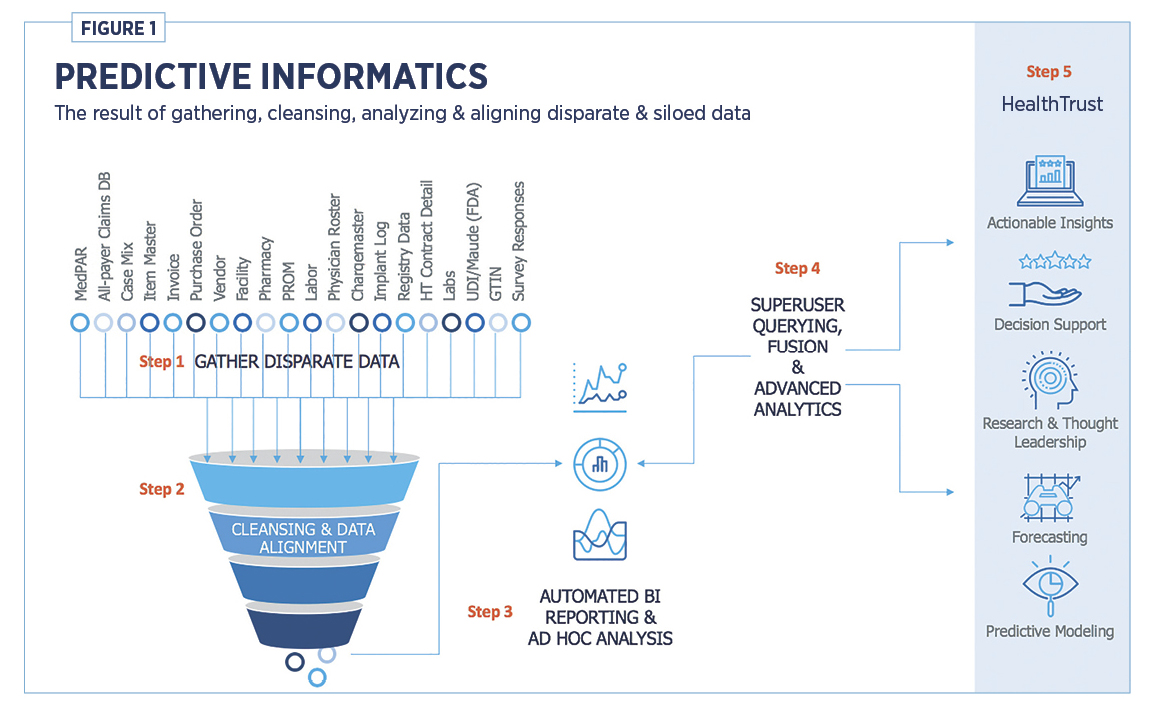
“Initially, our focus will be to provide clinical informatics for orthopedic, spine and cardiovascular service lines as well as pharmacy. We will expand into additional specialties as member demand increases,” Young explains.
HealthTrust is increasing its clinical informatics capabilities to:
• Consume and collate data from disparate sources in a variety of formats and disseminate it in uniform and user-friendly dashboards
• Deliver analytics to members across multiple platforms, including web-based and mobile applications
• Customize member dashboards to meet specific and unique needs
• Provide added value through predictive analytics and artificial intelligence
• Contract with an experienced partner to offer best practices and enhanced capabilities related to data security, data consumption, scalability and customer support. The goal is to be innovative, flexible and capable of meeting the evolving needs of the HealthTrust membership
At least two levels of dashboard access will be available to HealthTrust members, including key performance indicators and performance benchmarking at the IDN, division, regional and facility levels. An additional level of access will offer subscribers provider-level benchmarking and customizable dashboards.
A collaboration of Physician Advisors, internal subject matter experts and HealthTrust members (representing pharmacy and traditional provider service lines), was held at the end of 2018. Participants offered their insights on renovating HealthTrust’s clinical data and analytics solutions by identifying and prioritizing key performance indicators for each specialty and by outlining the data sources and dashboard requirements. HealthTrust member feedback will continue to shape the design and user experience of the informatics solutions moving forward.
Share Email Information Technology, Metrics and Tracking, Q3 2019






