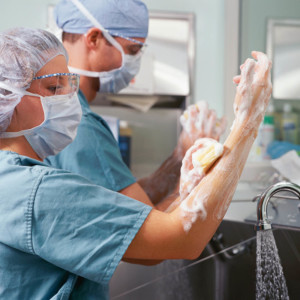
Enlist Supply Chain in the Hospital Infection Fight
One in 25 patients in U.S. hospitals acquires an infection as part of his or her care, according to a recent report by the Centers for Disease Control and Prevention (CDC). Those infections, which are sometimes lethal, commonly include pneumonia and those occurring at surgical sites and in the gastrointestinal tract, urinary tract and bloodstream. While the issue of hospital-acquired infections remains a stubborn and serious problem, many healthcare facilities are making strides to reduce infections—and supply chain professionals can play an important role in continuing that trend.
We continue to see decline in several infections nationally,” says Cliff McDonald, M.D., senior advisor for science and integrity in the CDC’s Division of Healthcare Quality Promotion. “In most cases, the specific types of products used are just as important in reducing infections as the procedures followed by healthcare practitioners.”
For instance, another CDC report recently revealed decreases in central line-associated bloodstream infections (CLABSI), which dropped 44 percent between 2008 and 2012. During this same time period, there was a 20 percent decrease in infections related to 10 surgical procedures tracked in the analysis.
Between 2011 and 2012, there was a 4 percent decrease in hospital-initiated MRSA infections. And during that timeframe, there also was a 2 percent decrease in hospital-initiated Clostridium difficile infections.
Making Progress
As the CDC and other groups research the most effective techniques for reducing hospital infections, systems across the country are making small changes that are yielding improved results. For instance, HCA participated in a recent study with the CDC, Harvard researchers and the federal Agency for Healthcare Research and Quality to help reduce bloodstream infections like MRSA in ICU patients. The study found that universal decolonization, or bathing patients upon admission with chlorhexidine gluconate (CHG), an antiseptic cleanser, and mupirocin, an antibiotic ointment, reduced such infections by 44 percent.
The study showed that CHG in a cloth formulation was most effective for preventing MRSA infections. So when the results were final last year, HCA began implementing baths with CHG cloths in ICUs at each of its 165 hospitals across the country, says Edward Septimus, M.D., HCA’s medical director for infection prevention and epidemiology. While the new practice means a significant increase in products that must be provided by supply chain professionals, the results have been powerful in terms of keeping patients healthy.
In addition to using CHG cloths to reduce MRSA infections, hospitals also have found success recently by using alcohol caps that fit over medicine ports. When the port is not in use, alcohol bathes the connector, a process that has been able to reduce infections. The use of these alcohol caps is the newest product-based approach to preventing infections, having been in practice only during the past year or so, Septimus says.
“It’s important to note that alcohol caps are considered a special approach and not a routine standard of care. But for hospitals to continue to see decreased bloodstream infections, their use may be an effective strategy,” he says.
To prevent infections caused by intravenous catheters, the combination of a large skin drape and certain substances used to prep the skin have yielded success. However, because all of these items used to be packaged separately, it was possible for practitioners to overlook one of the steps.
At HCA, supply chain professionals took a role in helping to reduce those infections by purchasing all the needed items for prepping and inserting intravenous catheters—such as a large skin drape, gloves and the needed antiseptics—in one package.
“So now these kits have everything necessary to help healthcare professionals make sure they complete each step,” Septimus says. “The infection rate is higher if you use a different type of skin preparation or make other slight changes, so when our supply chain professionals package everything together, that helps us do it right every time.”
For some infections, specific techniques in providing care are more important for preventing infections than the products used. For instance, in certain populations, some hospitals have been using silver bladder catheters in an effort to reduce urinary tract infections, Septimus says.
However, a more definitive study published in 2012 showed that silver catheters did not reduce the occurrence of symptomatic urinary tract infections. Instead, “it’s more important to focus on techniques such as hand-washing, inserting catheters only when needed and taking them out when they are not needed,” Septimus says.
Catholic Health Initiatives (CHI) also has made progress in decreasing infections. It has had marked success over the past three years in reducing CLABSI by using Biopatch, a cholorhexidine-impregnated sponge, almost universally across its hospitals, says Aaron Williams, national infection prevention director for the hospital group. After on-site infection control professionals establish evidence-based practices for reducing infection, such as using the Biopatch sponges, those practices are added into CHI’s Evidence-Based Practices Toolkit, a companywide online resource that provides the base level of guidelines and practices that should be followed to reduce infections, Williams says.
Involving the Supply Chain
Many of the recent successes in reducing hospital infections are reliant on the purchase of specific products that help prevent contamination. For instance, the landmark MRSA study couldn’t have been completed “without the supply chain having what we needed available to take care of every patient,” Septimus says.
However, the products that are most effective in keeping patients healthy aren’t always the most cost-effective ones. And implementing new products or changing orders to help fight infections can be a lengthy, difficult process. For that reason, it’s vital that supply chain professionals understand how their purchasing decisions may impact the lives of patients.
“It’s important for supply chain professionals to understand how they fit in as part of the team approach to healthcare,” Septimus says. “It’s more than a cost issue. If you look at it just from a financial perspective, it doesn’t make sense because [purchasing some of these products] raises costs. But by understanding the literature and which products are evidence-based, healthcare teams can come up with better outcomes, which makes the products cost-effective.”
At CHI, the materials management group formed a corporate-level Value-Based Purchasing/Infection Control Committee to facilitate coordination between product selection and clinical needs.
“The central principle of the team is patient safety at its core and how it aligns with need and good stewardship,” Williams says. “The group examines product types, need, processes and evidence in regard to larger overreaching areas of patient safety, use, efficacy and value-based purchasing reimbursement.”
After the committee makes a decision, its recommendations go through a structured process for endorsement. Currently, the group is examining daily CHG bathing of patients with central lines and alcohol impregnated hub caps. While the committee is relatively new, it aims to become a lasting partnership that will allow “a range of individuals who are experts in their own areas to collaborate on appropriate product selection to ensure patient safety,” Williams says.
Septimus says financial decision-makers should be involved from the beginning of a project to reduce hospital infections. If not, a product may go through the stages of observation and recommendation, only to be refused by a budget officer because it wasn’t included in the facility’s budget.
By taking a long-term view, hospital personnel can focus on the savings of infection prevention purchases, rather than the immediate costs. For instance, patients who leave the hospital with an infection may become disabled or require further hospitalization, which will result in further cost to society, if not the hospital itself.
“If we prevent a certain number of infections, not only are we saving lives, but we’re saving money as well,” Septimus says. “There’s a societal cost that is much greater than the monetary cost of preventing infections. Yes, there will be a cost in terms of what we’re investing, but our outcomes and revenue will improve, and we’ll be saving lives. Even though there may be a blip in our operations in the short term, it will be well worth it in the long run.”
Share Email Hospital Acquired Infections, Infection Prevention, MRSA